Advances in lighting and control technology are paving the way to more comfortable lighting that is intuitive and efficient for patients, their families and their health care providers
Learning Objectives
- Design advanced lighting control solutions for health care projects to improve comfort, simplify control and make facilities more future proof and energy efficient.
- Become familiar with lighting control strategies and application-specific considerations for health care projects.
- Understand power structure in a typical health care facility — nonessential, life safety and critical — and how it affects the desired sequence of operations.
- Use today’s modern fixtures and control systems to offer a broad array of solutions that can give patients, their families and health care providers more control while elevating the overall experience of the space.
Over the past few years, health care facility design has become more focused on the patient experience. Two important and emerging trends supporting this evolution include giving patients more control over their environment and implementing flexible technologies that adapt over time to meet changing health care needs. Designing advanced lighting control solutions into health care projects can improve comfort, simplify control and make facilities more future proof and energy efficient at the same time.
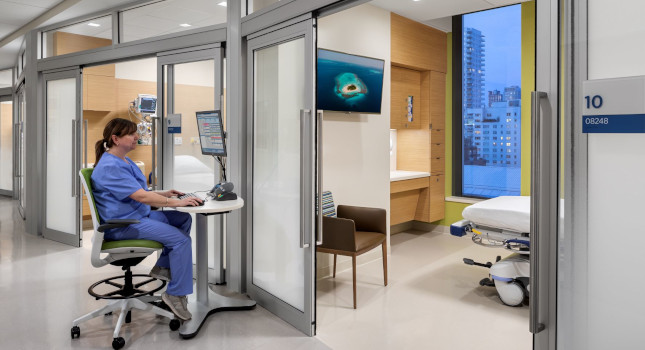
Because patients spend most of their time and interact most heavily with providers, staff and technology in their hospital rooms, the patient room is a focal point of lighting design. Lighting can play an important role in creating a more inviting atmosphere, giving both the patient and the provider control over the mood, atmosphere and functionality of the space. Lighting that is more personal and accessible helps transform the room from a primarily clinical, sterile environment to a space that helps put patients and their families at ease.
While primary focus is on the patient, a positive experience is also critical to everyone who uses the space including nurses, doctors, other clinicians and hospital staff. How can you design lighting and control to best serve everyone’s needs?
With a well-designed system, the patient can turn off over-the-bed lights to take a nap, while visiting family members have enough light to read. With the press of a button, a nurse can do middle-of-the-night bedside checks under dim light that reduces stress on the patient; touch a different button and all lights can come to full for an exam or emergency situation. The key is to enable the right light at the right time.

How power interfaces with the lighting
Before getting into the details of a lighting control system, it is important to realize that power in a health care facility is different from power in a typical commercial space (for complete details, visit NFPA 101: Life Safety Code). Rather than normal and emergency feeds, there are nonessential and essential power feeds. Nonessential power is the same as normal power in a standard commercial building. Essential power is made up of a life safety branch, similar to the emergency backup power in a typical commercial building, intended to support safe egress, as well as a critical power branch to keep hospital operations working normally under emergency power.
How the lighting control system interacts with these power systems deserves further explanation, starting with the critical power branch. Lights always function in the critical branch of the essential power feed. They continue to operate as they are programmed, with no lockout and no override, even under backup power and are used in areas such as operating and patient rooms that must stay functional during a power emergency.
During the loss of utility power, devices on the critical branch continue operating, uninterrupted and unchanged, for patient safety and support. Emergency room lighting, for example, can’t just default to standard egress levels (often 100%); it must maintain the lighting level at the time of the power loss.
The life safety branch, on the other hand, is analogous to emergency power in a standard commercial building. These loads include exit signs and egress lighting and they are subject to lockout and override to maintain minimum light levels in an emergency allowing occupants to quickly and safely, exit the building. Nonessential or normal power is used for the remaining noncritical, nonlife-safety lighting and equipment.
From the specifying engineer’s perspective these circuit requirements and the need to account for three separate power feeds mean it is important to think about lighting early in the planning process. Patient rooms may have all three branches feeding them, but not all three branches may be used with the lighting control system. It is common for only the critical and nonessential feeds to be used with the lighting system in a patient room. The life safety feed is often used only with a stand-alone emergency/battery backup fixture.
Multiple power feeds can complicate the installation as well. For example, the lighting design cannot mix the different power branches in the same junction box or in the control panel without proper separation and the definition of proper separation depends on the type of control protocol being used. For a 0 to 10 volts system, for example, you may need independent controllers for each power source.
For digitally controlled systems with addressable drivers, you can generally mix the control wires from different power sources without special barriers because the line voltage typically goes direct-to-fixture rather than to the controller.
However, the controller itself should be on the critical branch. Fixtures on a digitally controlled system may be entirely on the critical branch, but sometimes there may be some stand-alone light switches or dimmers on the nonessential feed.
A typical sequence of operations might look like this:
- Nonessential branch lighting operates as programmed when utility power is present. Lights must turn completely OFF when utility power is not present.
- Life safety branch lighting loads will be powered when utility power is present, can be turned ON or OFF at any time and can function as part of a system. When utility power is not present, life safety loads must meet minimum light levels in specific areas in the hospital, primarily for egress purposes.
- Critical branch lighting must function the same way regardless of utility power or backup power. For example, consider emergency room or operating room lighting — you would never want to lose control of your lights midsurgery, whether a generator or utility power is supplying the room lighting at the time. You just need the lighting to work as programmed.


Characterizing patient room design and layout
Despite their relatively small footprint, patient rooms accommodate many users and a wide variety of functions. A typical space this size usually has only one or two lighting zones, but a hospital patient room will often incorporate between four and 12 lighting zones. This zone density, together with the complexity of the different branch circuits, requires careful planning. Power, controllers and keypads all need to be coordinated early in the design process.
Lighting zones in a patient room are usually divided between three to five main areas:
- Patient/bedside area — Often this comprises two-to-four zones of light in a specialized, over-the-bed fixture and may also include shade control.
- Family/sitting area — Typically along the outside wall, this may include one or two zones of independently controlled lighting.
- Nurses’ station/sink area — This may be broken into different lighting zones for a small desk/work area, exam lighting and room entry light.
- Bathroom area — Often has at least two zones of light for patient safety and comfort.
- Entrance area — Generally a single switched light.
A typical layout features different power feeds and voltages — 277 volts critical, 120 volts nonessential and 120 volts life safety are all represented in this lighting design example. Critical and life safety may have the same symbol on the reflected ceiling plan showing they receive backup power.
Reference the power plans to be certain whether the “emergency” designated fixture is fed from critical or life safety. It is also worth highlighting the battery-backup emergency fixture in the bathroom, which may not get controlled by the system or have local control, depending on the design of how that life safety branch is handled.

Benefits of digital control protocols for lighting
On today’s typical commercial project, it’s easy — and often standard — to specify analog, 0 to 10 volts control, which provides hard-wired zoning that most designers and contractors are familiar with from other applications where the wiring defines the functionality (all fixtures that are wired together get controlled together). However, the high-density zoning requirements in patient rooms make digital control, where a single control panel could manage as many as 128 zones, an attractive consideration.
When overall material and labor costs are factored in a system that uses individually addressable, digital control methods — such as DALI, EcoSystem or wireless protocols — can be the less expensive, higher performance alternative. With individually addressable fixture control, you need fewer control boxes, less conduit, less wiring and less time coordinating the lighting spec.
The sequence of operations in patient rooms can be advanced, with different lighting control scenarios required for patients versus care providers. These sequences require careful planning and often need multifixture control that is not easily accomplished with an analog solution. Analog wiring requires you to know the exact sequence at the outset of design, which can be unrealistic. A digital solution allows easy adjustments and rezoning, with no need to rewire, even after the space is in use; you can simply reprogram using software rather than calling an electrician.
Beyond capital expenditure savings, a digital control system can provide additional benefits. Flexibility and resilience have moved into the spotlight over the past few years. Many hospitals had to quickly adapt in the wake of COVID-19. In some cases, larger spaces had to be quickly subdivided to create individual patient room or isolation spaces. Capacity for patient care was compromised when spaces could not be easily reconfigured. For example, isolation rooms that are traditionally distributed throughout the hospital had to be consolidated in one area to ensure limited staff were able to provide necessary care.
A digitally addressable lighting control system can make it easier to redesign hospital spaces, allowing simple reprogramming of lighting zones to suit changing needs without the cost of rewiring a 0 to 10 volts lighting control system. Even the use of wireless control systems, historically excluded from health care applications, has seen broad adoption in many hospitals over the past few years, enabling greater flexibility and lower installation and reconfiguration costs.
Moreover, the medical staff may see the need to adapt the lighting overtime. As they learn their own teams’ behaviors and patients’ needs, the flexibility and simplicity of digital control offers the ability to intuitively make those changes as frequently or infrequently as necessary.

Having control over lighting
Why is there now so much focus on patient-room lighting? In a September 2021 Illuminating Engineering Society industry webinar, health care lighting design experts noted that during the COVID-19 pandemic, many people felt a loss of control over their own life situations and this gave providers and design professionals a new window of understanding about what patients may go through during a hospital visit. Patients and their families often deal with feelings of sacrificing control when they enter the hospital.
Giving them back some control over their environment, whenever possible, can lead to a better experience. Whether that’s the simple ability to dim or brighten lights in the room, use motorized shades to adjust the amount of natural light or even control the color temperature or brighten the room with saturated color, today’s modern fixtures and control systems offer a broad array of solutions that can give the user more control and elevate their experience in the space.
Researcher Andrea Wilkerson, lighting engineer/researcher for Pacific Northwest National Laboratory, and Brooke Silber, associate principal director of lighting for BR+A took part in the September IES webinar, and we share their timely insights here.
A study from 2020 points to the positive impact of light on behavioral health patients. Researcher Wilkerson is currently studying data in a behavioral health facility in which she is observing the number of times a patient adjusts his or her lighting. “We are getting objective data that helps us better understand a person’s mental health, behavior and progress,” said Wilkerson.
“Providing control in a behavioral health setting is empowering,” said webinar panelist Silber. “Lighting plays an important role in creating this inviting atmosphere by setting appropriate moods at the appropriate time, facilitating enhanced comfort, and maintaining a high quality of care.”
While top-priority focus is given to patients and their families, specifiers need to consider all the people who use the space including nurses, doctors and other clinicians. What are their needs and how do they use lighting and controls? As researchers focus on the patient experience, it’s becoming easier to discern specifically how a space is used and what each stakeholder needs.

Lighting hardware considerations
When it comes to controls in the space, patients and visitors need simple, intuitive control — akin to familiar residential controls — because that’s what they are used to. Hospitalization can be disorienting enough without having to figure out how to do something as simple as turning on the lights in your room. Intuitive zone control, with familiar on/off buttons, potentially with raise/lower options, is best. If the room incorporates motorized shading for natural daylight, you’ll also want to ensure those controls are obvious and simple to understand.
In contrast to patients, the doctors, nurses and staff use the space daily and can quickly learn advanced lighting control settings. Here, scene control can be extremely useful — a single touch to adjust lights and shades together can offer efficiencies to the care team. These scenes can be aligned with the typical tasks the medical staff perform, allowing them to complete them more efficiently — including evening check-ups, daytime exams or an urgent emergency.
Manufacturers offer a variety of control types that can easily be mixed and matched to serve the needs of both patients and medical staff. Choosing the right combination of controls goes back to a familiar theme — start planning early and carefully consider the sequence of operations.
Bedside control is its own area of consideration and it typically centers around the pillow speaker. A pillow-speaker is a handheld remote control that allows a patient to call a nurse or control many things in the room including the TV, motorized shades and lighting without leaving the bed. The key to pillow speaker control is coordinated integration between the lighting control and pillow speaker manufacturers.
Integration methods can vary between simple contact-closure to more sophisticated network-based integration. Work with your selected vendors to get the desired functionality and the right control configurations, worked out. Like the wall keypads, simple control configurations are essential since many patients have little or no previous experience with these hospital-specific controls. Zone control that toggles a light on and off, easily indicated on the pillow speaker by a simple light bulb icon, is typically a great option.
Ensuring a lighting project’s success
When lighting designers start a project, they should get the stakeholders together and define goals and budget up front for the greatest impact and to fully understand how the client expects the lighting control system to behave. Consider all the expected use cases and develop your sequence of operations based on that information. In today’s projects, stakeholders often include some nontraditional players, such as IT departments that have concerns about cybersecurity, integration or remote access.
Another common practice in hospital design is to create a full-scale working mock-up of the room, invite stakeholders into the space and ask them to provide feedback based on a hands-on experience rather than just a hypothetical one. This often leads to better outcomes and fewer concerns once the final space is installed and operational.
Properly identifying application and stakeholder requirements is key to a simple, flexible lighting system that can make a positive impact and ensure long-term satisfaction. Starting with a well-designed specification helps to ensure that installation, programming and potentially reprogramming of lighting systems are as simple as possible, while providing patient and staff-friendly solutions that meet the ongoing needs of the institution.



