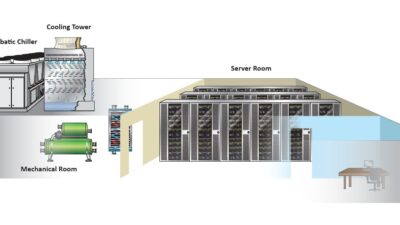
As hospitals and health care facilities evolve, the HVAC systems within them must update to meet air quality and HVAC needs

Hospital, health care insights
- Hospitals, health care facilities and related medical buildings are changing HVAC systems to meet the needs of resiliency, new outpatient facility demands and energy efficiency.
- Additional air filtration is often designed into the hospital HVAC system.
Respondents
- Tanner Burke, PE, Senior Fire Protection Engineer, ACS Group, Austin, Texas
- Derek Cornell, Senior Associate, Certus Consulting Engineers, Dallas, Texas
- Beth Gorney, PE, Assistant Project Manager, Dewberry, Raleigh, North Carolina
- Sierra Spitulski, PE, LEED AP BD+C, Associate Principal/Studio Leader/Mechanical Engineer/Project Manager, P2S Inc., Long Beach, California
- Kristie Tiller, PE, LEED AP, Associate, Team Leader, Lockwood Andrews & Newnam Inc. (LAN), Dallas, Texas.

How have you and your team addressed the unique air requirements of COVID-19?
Derek Cornell: In hospitals, the approach to HVAC systems in response to COVID-19 has evolved through stages of the pandemic. The additional exhaust and outside air required poses obvious challenges in existing facilities. The more difficult challenge has been designing for flexibility to help ensure prescriptive health care code compliance, maintain environmental conditions and minimize additional energy consumption outside of pandemic surges and state/federal disaster declarations.
For example, in smaller hospitals with existing systems limited in the ability to handle additional outside air load, strategies such as HEPA fan-filter units ducted back into the return system help to minimize the need for major system upgrades and also provide flexibility in returning to normal pressure relationships outside of a pandemic.
Kristie Tiller: We’ve had a lot of discussion regarding air cleaning products being installed at the suggestion of the manufacturers. UV lights and Ionizing filters, for example. Some building owners are arbitrarily increasing the amount of outside air in their buildings. The guidelines from the various agencies are still in flux and it’s difficult to know which modifications can be made that are both sound investments for health and safety and capital expenditures.
Sierra Spitulski: For one recent project, we were asked to create a pandemic ready pod within the emergency department for highly contagious patients. To protect the staff and nurses working around patients, computational fluid dynamic modeling of air distribution was performed on a typical emergency department scenario. This allowed us to design the HVAC distribution in a way that optimized infection control which can help reduce spread of disease and illness.
How have you worked with HVAC system or equipment design to increase a building’s energy efficiency?
Sierra Spitulski: We work with health care providers, builders and designers to create reliable, energy-efficient facilities that safeguard their patient’s health and comfort while simultaneously reducing operating costs. Lately, we’ve been leveraging current code exemptions to decrease airflows in specific areas of the hospital during unoccupied hours through strategic zone level controls, finding creative ways to decarbonize such as rejecting boiler fuel heat to raise the temperatures of the domestic hot and heating hot water systems, in addition to more obvious decarbonization efforts such as heat recovery chillers and electric boilers. Specifically designing the air handlers to be dual duct and dual mixing box has also shown an incredible amount of energy savings in a system.
What is the most challenging thing when designing HVAC systems in such buildings?
Kristie Tiller: The most challenging HVAC design in health care tends to be renovations in active facilities. Renovations are never simple, especially in older buildings, due to existing structure, utilities and equipment location. In an active health care facility, it is especially important to maintain proper conditions while phasing from the old equipment to the new. As engineers, we must work hand in hand with the contractors to ensure that we maintain the health and safety of the patients while renovating existing systems. This includes proper selection of equipment type and location, the right temporary equipment and careful phasing of construction.

Sierra Spitulski: Challenges are abundant when planning HVAC for hospitals. Equipment that is seismically certified in California comes from a much smaller pool of resources and is not always readily available. Long lead times for this specialty equipment impacts construction schedules, cost and facility cashflow. Infection control protocols and limitations to shut down times require detailed construction procedures. Then, when the new equipment is being installed in a live 24/7 acute care hospital, it’s often necessary to have an engineer in the field with the contractors to assist with troubleshooting as the room for error is small–and this is likely happening in the middle of the night.
What systems are you putting in place to combat hospital acquired infections (HAI)?
Derek Cornell: In the aftermath of the pandemic, a cleaner environment for patients and staff is ever-increasing and with that, we have seen a trend in UV technology. The use of UVGI (ultraviolet germicidal irradiation) lamps in air streams, while not new technology, are gaining popularity. UVGI lamps in air streams has been pretty popular over the past couple of decades, however, newer technology using UV-C LED lamps is now becoming prevalent in light of recent years. These are replacing the older mercury UV lamps. We are also seeing them applied for more effectiveness using higher watts/square foot irradiation intensity.
Sierra Spitulski: State and federal code regulations and recommendations for hospitals already contain elements aimed at improving air quality and removing airborne pathogens: low-level air exhaust near a patient’s head in infection-control spaces to remove exhaled particulates from the airstream, multistage filtration at the air handling unit, negatively pressurized and exhausted dirty spaces and positively pressurized and HEPA-filtered protective spaces for the most vulnerable and immunocompromised patients. Hospitals can opt-in to additional levels of HVAC cleanliness through the use of UV lights in the air handling system to further eradicate airborne pathogens, increased levels of MERV filtration and regular maintenance and cleaning. There are also lots of conversations and constantly evolving research around recommended airflows over and around patients in an operating room environment.
What type of specialty piping, plumbing or other systems have you specified recently?
Sierra Spitulski: Our team is on the cutting edge of today’s medical advancements. This includes codes, standards, new technologies and California Department of Health Care Access and Information (previously OSHPD) requirements. There’s a new requirement in California that’s hitting all hospitals in 2030 that will require all acute care facilities to provide on-site storage for 72-hours or more for domestic water, waste water and emergency generator fuel oil. These requirements are aimed at enabling hospitals to maintain functionality in the event of a disaster that renders the city services inoperable for a period of time. This is a massive undertaking, as this means anywhere from 10,000 to 100,000 gallons worth of storage for these resources, which can be an even bigger challenge in landlocked hospitals.
Medical gases are vital for hospitals and medical campuses. Define the project, its goals, the challenges and the design solutions.
Tanner Burke: We provided consulting on the code challenges for medical gas upgrades to a Level 3 imaging room at a medical facility in Northern Nevada medical facility. This involved review of the 2018 Facility Guidelines Institute and NFPA 99: Health Care Facilities Code requirements to determine the required quantity and location of medical gas outlets, as well as the provisions associated with the medical gas zone valve box nurse alarm systems.
Derek Cornell: The need to design medical gas systems for increased ventilator quantities is here to stay. We are currently working on a full evaluation and design of upgrades to a large campus oxygen (O2) system. At this facility, one of the largest COVID surges occurred simultaneously with extreme winter conditions for the region, resulting in adverse road conditions making increased frequency of deliveries difficult. In the extremely cold weather and very high demand, icing of the vaporizer was also an issue. The proposed design includes a complete replacement of the bulk O2 system in a new location while keeping the existing hospital operation via connection to multiple emergency oxygen connections.