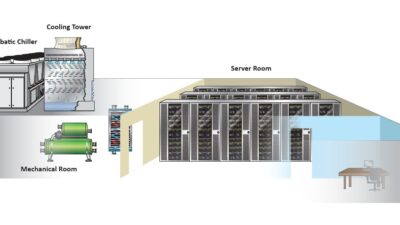
Stand-alone medical buildings and specialized treatment facilities are engineering challenges, and more are being designed and built due to changes in health care requirements. Codes and standards dictate much of the design of these facilities.

Respondents
Neal Boothe, PE, Principal, exp, Maitland, Fla.
Douglas T. Calhoun, PE, Senior Vice President, WSP | Parsons Brinckerhoff (formerly ccrd), Dallas
Caleb Haynes, PE, Principal/Director, TME LLC, Birmingham, Ala.
Brian Kolm, PE, Team Leader, Mechanical, HDR Inc., Omaha, Neb.
Craig Kos, PE, LEED AP, Vice President, Environmental Systems Design Inc., Chicago
Bryan Laginess, PE, LEED AP, Vice President, Peter Basso Associates, Troy, Mich.
CSE: How has the Affordable Care Act changed your approach to the design/engineering of these buildings?
Kos: Who owns and operates outpatient facilities has changed along with expectations on how they will perform. The Affordable Care Act was a catalyst for health care systems to move more diagnostic and treatment procedures to these buildings. Doctors are sharing spaces to a greater degree. We see increased attention on limiting construction costs. There are expectations for increasingly shorter construction phases. All the while, the end user still wants the highest quality and increased flexibility.
Kolm: Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) scores are focused on patient satisfaction. Designing communication infrastructure and communication devices with integration in mind is the basis of the necessary flexibility for decisions made during the life of the building. Minimizing the number of cabling solutions can save construction cost, for example; connecting a Category 6 (or 6A) to a television in lieu of coaxial cable saves the owner both in cable costs and enables one contractor to complete the work in lieu of two contractors. Integrating the television with meal ordering, room-temperature control, movies, educational channels, and review of physician’s orders provides patients with the flexibility they expect, and potentially better HCAHPS scores for the health care facility. These decisions on infrastructure and integration need to be discussed early in the design process in an attempt to "future-proof" the facility.
Haynes: With Medicare reimbursements now tied to patient satisfaction through HCAHPS scores, we’ve brought an increased focus on the patient experience into our designs. Most engineers think of their systems as out of sight, out of mind; they are, as long as they are working. But we have tracked studies that link most patient transfers to failed components of the engineering design, and each transfers costs the hospital around $400 to $500. We can have a significant impact on the facility’s bottom line with respect to operability and the durability of our systems.
CSE: How has the convergence of automation and controls affected the design of stand-alone medical buildings and specialized treatment facilities?
Kolm: The convergence of automation and controls has allowed engineers to push the envelope of mechanical design by improving energy efficiency. Through variable speed drives operating fans based on static pressure in the duct system, to resetting the air changes to a space based on unoccupied periods, these energy-saving control strategies would not be so commonplace without the use of integrated automation and control design.
CSE: Please explain some of the codes, standards, and guidelines you use as a guide. Which codes/standards should engineers be most aware of in their design?
Calhoun: Facility Guidelines Institute (FGI) guidelines, state health-department guidelines, international codes, and state boiler codes are key. For medical facilities, engineers should be particularly aware of the state health requirements and those that apply or do not apply to specific stand-alone facilities, depending on licensure.
Laginess: Aside from the International Code Council (ICC) codes, states may have their own health care facilities guides that they will enforce. We have the Minimum Design Standards for Healthcare Facilities in Michigan. It has many similarities to the AIA Guidelines for Design and Construction of Health Care Facilities. ASHRAE also has several health care facilities resources.
Haynes: There are multiple codes and standards that must be taken into consideration. Ultimately, the codes that are used are dependent on the ones that enforced by the authority having jurisdiction (AHJ). Some of these codes include ICC, NFPA, those issued by local and state health departments, etc. Industry standards and guidelines that need to be considered include FGI, ASHRAE, U.S. Green Building Council’s LEED, Veterans Affairs design guides, etc. In addition to codes, the engineer must consider CMS requirements for Medicare and Medicaid reimbursement and insurance requirements, such as FM Global, to ensure that the building is insurable at the most reasonable rate.
Kolm: One would consider the FGI Guidelines as the publication to follow to design a stand-alone medical building correctly—from the layout of the spaces to the engineering design requirements for the facility. In addition to the FGI Guidelines, the standard to follow, mechanically, would be ASHRAE Standard 170: Ventilation of Health Care Facilities and its associated addenda. This document lays out a framework on how to design certain spaces within a medical facility, from the required air changes, temperature/humidity of the space, diffuser type to use, and the required pressurization of the space.
Boothe: Most codes that apply to full hospitals also apply to these outpatient medical facilities, but often there are some reduced requirements. For example, the FGI guidelines have separate sections for outpatient facilities, freestanding outpatient diagnostic and treatment facilities, primary care outpatient centers, etc. In these sections, there are still specific requirements similar to hospitals, but they are often not as severe. Other health care codes such as NFPA 99: Health Care Facilities Code and NFPA 70: National Electrical Code (NEC) Article 517 still apply to these facilities, too, as they are still serving patient-care areas. You also have to be aware that many states have their own health codes in addition to the national building codes.
Kos: We need to comply with all state and local building codes while understanding the implications of the new (not-yet-adopted) NFPA codes as they relate to the Department of Health and Human Services and to future CMS requirements. Additionally, energy codes continue to get more stringent, necessitating owner education and budgeting to implement. HIPAA regulations address security and privacy of protected health information. This regulation also highlights acoustic and visual privacy. The Americans with Disabilities Act applies to all public facilities and greatly impacts building design with its general and specific accessibility requirements. It is also important to understand owner guidelines because they are becoming increasingly stringent as hospital owners push into outpatient facilities.
CSE: How have International Building Code (IBC), Joint Commission, NFPA, ASHRAE, and other codes affected your work on such projects? What are some positive/negative aspects of these guides?
Kolm: These codes have aided in the standardization of designing health care spaces for engineers and architects over the years; particularly the FGI guidelines and ASHRAE 170. The majority of what comes from ASHRAE 170 is based on research and data collected from ASHRAE that validates design criteria to not only keep patients safe from infections and the spread of disease, but to protect staff as well. However, the FGI guidelines and ASHRAE 170 are not the only governing documents in the design of health care spaces. Documents such as NFPA 99, the IBC, the U.S. Pharmacopeial Convention 800 Guidelines, as well as the Association for the Advancement of Medical Instrumentation Standards for Sterile Processing Departments are also available for particular areas of health care designs. Some aspects of these documents can be contradictory to each other, which can lead to confusion for the architect, engineer, and owner as to what to follow. In terms of health care design, it would be beneficial for these organizations to join forces and come up with one document for the designing of health care spaces.
Kos: For ambulatory buildings, the rules and regulations from these entities are the minimum standard of care and the basis of the AHJ review. For medical office and other clinical spaces, they can create issues because they haven’t caught up to the evolving outpatient model with varying degrees of clinical intensity. If hospital and ambulatory design practices and codes are applied to all clinical spaces without discrimination, they can contribute to overcomplicated designs that are costly to install and operate. When working with hospital systems, the design process should include meetings with the clinical staff and infection control to determine the procedures and level of patient risk, so that appropriate system design can be applied.
Laginess: There are a lot of codes and governing bodies on these projects. Everyone wants to build a quality, safe environment for the patients and staff. The codes and guidelines help by defining the minimum needs of the facility, but occasionally we’ll run into a situation where the same topic is addressed by more than one jurisdiction, and we’ll have to make sure we are designing to the most stringent language.
Haynes: The convergence of the applicable health care codes-and more importantly, their divergence-has a significant impact on the skyrocketing costs of health care. The financial burden of conflicting code bodies and improper interpretations has burdened the first cost and lifecycle costs of health care facilities across the nation. I would encourage anyone interested in health care governing codes to get involved in the sponsoring organization and make your voice heard.
Boothe: All of these mentioned national codes and standards affect the design of outpatient health facilities. One area that requires care is in reviewing all these codes, as sometimes they have different requirements that may conflict with each other. When this happens, the most stringent should be followed. For example, both NEC Article 517 and NFPA 99 have requirements for how many electrical receptacles are needed in patient-care areas. Sometimes, NFPA 99 requirements exceed those of NEC Article 517 in quantity of receptacles. Meeting the quantity of receptacles per NEC would not necessarily meet the requirements of NFPA 99.