The Bala Consulting Engineers COVID-19 Task Force has published a white paper to assist engineers in making buildings safer
The COVID-19 virus has forever changed our perspective on cleanliness, personal interaction and our environment. The thought of a post-pandemic state brings us hope. But what does a post pandemic environment look like and how does it operate? Bala has researched and collaborated with industry partners and health experts to present some of the most effective ways to make our buildings safer. From filters and air changes in HVAC systems to sanitization and touchless toilet fixtures as well as technology integrations for access control and bio-scanning, there are short and long-term strategies building owners can implement to increase the safety of their building. These building systems strategies, coupled with architectural strategies, will reassure occupants that the buildings they are returning to have evolved to keep pace with the latest in health and safety guidelines.
Our recommendations can be found in the COVID-19 Insights area of our website. They are based on the research conducted by our team of engineers. This research continues as the data and knowledge on COVID-19 evolves. We will update this report when we have new information to share.
The virus
COVID-19 (or 2019-nCoV), as named by the World Health Organization (WHO), is the disease caused by the new coronavirus that emerged in China in December 2019. COVID-19 is caused by the SARS-CoV-2 virus. As a result, parallels are being drawn between the 2003 SARS outbreak and the spread of COVID-19.
Coronavirus gets its name due to the crown shape of the virus.
Researchers know that the new coronavirus is spread through direct contact with an infected person or by touching a surface or object that has the virus on it and then touching your eyes, nose, or mouth. It can also be spread through larger droplets released into the air when an infected person coughs, sneezes or talks. The droplets generally do not travel more than six feet, and they fall to the ground (or onto surfaces) in a few seconds. Although a study by NHK Japan and its researchers found that resultant micro-droplets can stay suspended in the air for a long time, researchers from John Hopkins Health System are not 100% sure if these smaller droplets can carry the virus and suspend it in the air for longer distances. Therefore, some experts are recommending a more conservative approach that includes maintaining longer distances between people.
According to a new study from National Institutes of Health, CDC, UCLA and Princeton University scientists in The New England Journal of Medicine, scientists found that severe acute respiratory syndrome coronavirus (SARS-CoV-2) was detectable for up to three hours in aerosols, up to four hours on copper, up to 24 hours on cardboard and up to two to three days on plastic and stainless steel. The incubation period (or when symptoms appear) is within 14 days of exposure. As a result, staff members can be in the workplace and not even know that they are infected. Additionally, new research from China indicates that the novel coronavirus is also spread by fecal-oral transmission.
In rare cases, COVID-19 can lead to severe respiratory problems, kidney failure or death.
Early information out of China, where the COVID-19 outbreak began, shows that some people are at higher risk of becoming very sick from this illness. Those include:
- Older adults, with risk increasing by age.
- People who have serious chronic medical conditions such as:
- Heart disease
- Diabetes
- Lung disease.
Most experts agree we should take precautionary steps when facing possible contact with people or surfaces that may harbor COVID-19. These steps include:
- Personal protection equipment (PPE) – predominantly masks and gloves
- Isolation – maintaining safe distances between people and between people and contaminated surfaces.
- Cleaning/disinfection.
In summary, COVID-19 is a new highly contagious virus that predominantly spreads through contact and dispersion of droplets between people and nearby surfaces. Because of this contagion level, as people return to the workplace we will need to take these precautionary steps for personnel, furniture, and HVAC and plumbing systems. These measures will need to be put in place until a vaccine is discovered, but possibly beyond due to the aggressive nature of the virus.
HVAC solutions
Controlled access, separation and cleaning represent the some of the primary defenses against the spread of the virus. However, protections may be applied to existing and new HVAC systems to minimize further spreading of the virus within the workplace.
Several measures may be adapted from practices that healthcare and Bio-Safety Level (BSL) research facilities use to protect staff. It must be noted that measures applied to infectious disease rooms, BSL laboratories and clean spaces are designed for specific applications under highly controlled environments and access.
Clean rooms control particulate of specific sizes and rely on laminar airflow within the space to minimize recirculation of contaminants and to promote capture. Clean rooms require airflow injected high across large areas of the ceiling and discharged at low velocity to direct airflow down to low returns located at the perimeter of the spaces. Modifying HVAC systems to a similar configuration for office spaces would be extremely expensive. Furthermore, if staff are required to wear protective masks and they are unknowingly infected, the masks will capture the majority of virus that cling to droplets that are released with normal breathing or sneezing.
BSL facilities utilize similar methods with the distinction that highly contagious microorganisms are restricted to sealed environments such as isolators and glove boxes within the protected environment.
Another feature of these facilities is that they are designed to capture and contain particulate or vaporized droplets that may hold the contaminants such as the coronavirus. To be effective, the exhaust or return inlets need to be placed within proximity of all potential contamination sources noted previously. As noted within the American Conference of Governmental Industrial Hygienists Industrial Ventilation Guideline, the velocity of the airflow at an inlet will exponentially decrease with the distance from an inlet, as demonstrated within the figure in the link here American Conference of Governmental Industrial Hygienists Industrial Ventilation Guideline. As the velocity decreases further from the inlet, its ability to suspend and capture particulate greatly diminishes.
Since it is not practical to install exhaust or return capture points within inches of each person so that they pull contaminants away from a person’s breathing zone, we must look to adopt other measures that are similar to healthcare and BSL practices and apply them to the office workplace. Effective measures include:
- Installing filtration (antimicrobial filters, HEPA), bi-polar ionization and UV lights at return air openings and at components within the air system
- Implementing pressurization control and/or enhance current practices
- Increasing airflow (recirculated and outside air)
- Deactivating demand control systems that limit concentration of outside air
- Operating systems longer and with higher outside air content to flush spaces due to increased use of cleaners
- Operating ventilation systems serving communal spaces such as toilet rooms continuously (24 hours/day), since they have a higher risk of contamination
- Maintaining minimum relative humidity levels
- Sanitizing ductwork with aerosol sprays or UV light
- Using portable air purifiers.
Filtration
For any particulate that is captured and pulled into the HVAC system, filtration may be effective if properly applied. First, understand that the size of the coronavirus (as well as all viruses) is very small and will pass through almost all filters if independently suspended in the airstream. Refer to figure in this link. However, filters will intercept larger particulate that may contain the coronavirus. It is understood that the virus will attach to airborne particulate such as dust, which are captured by the high efficiency filters. The efficiencies of the typical HEPA filter is based upon particles at 0.3 micron. Note, HEPA filters and higher efficient ULPA filters will still capture a percentage of particles smaller than 0.3 microns. Also, the efficiency of these filters will improve as they become loaded, so it is not desirable to constantly change these filters. The main disadvantage to utilizing HEPA or ULPA filters in an existing HVAC system is the high pressure drops of these closely weaved filters. To minimize the pressure drop and the impact to an existing fan system, lower depth HEPA filters may be utilized. Another option would be to add booster fans to accommodate the higher pressures.
To further enhance the effectiveness of filters, it is advisable to utilize filters with antimicrobial coatings. Filters may be treated with antimicrobial coatings to kill dangerous microbes on contact.
Bipolar ionization
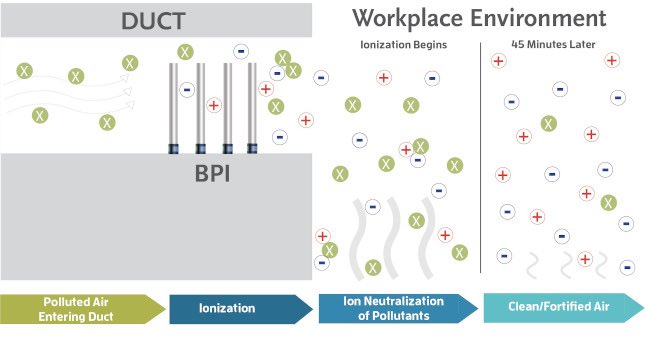
This technology releases positive and negative ions into the airstream as noted in Figure 1. Air flows along the ionization tube and oxygen from the air is charged to form ions. The ions are attracted to airborne particles like dust, smoke, VOC’s, allergens and other air pollutants. The ions latch onto and neutralize any contaminants they come into contact with. Charged particles are drawn together, forming clusters, which become heavy enough to drop out of the air. These ions work to deactivate single-celled, carbon-based organisms such as fungi, viruses and bacteria, whether they’re in the air or resting on surfaces. Note, this technology does not remove the contaminant but will help the enhanced filtration system capture the contaminant. This system will require vigorous cleaning procedures of all surfaces within the workplace environment as previously noted. To be effective, it is recommended that this technology constantly operate to maximize effectiveness.
UVC light
Application of UVC lamps at strategic locations within the duct system will kill microorganisms in the airstream (see Figure 2). However, placement is important since the coronavirus must be exposed for a period of time, which requires multiple UVC lamps within the airstream. Manufacturers are recommending exposure of 10 seconds within proximity of the UVC bulb, with some suggesting lamps every 6 inches.
Properly applied, UV lamps may reduce active coronavirus up to 90%.
Placement at each return air inlet would require multiple lamps, but that may be desirable for systems shared by multiple tenants. Other areas include locations that may trap particulate containing the coronavirus. These include sound attenuators, filters, energy recovery wheels, coils, and fans. However, if effectively applied, it may only be necessary and cost effective to treat one specific location within an air handling unit.
According to a 2018 report published by Scientific Reports (Volume 8, Article Number:2752), airborne-mediated microbial diseases such as influenza and tuberculosis represent major public health challenges. A direct approach to prevent airborne transmission is inactivation of airborne pathogens, and the airborne antimicrobial potential of UVC ultraviolet light has long been established. However, widespread use of UVC Light in public settings is limited because conventional UVC light sources are both carcinogenic and cataractogenic. It has been determined that far-UVC light (207–222 nm wavelength) efficiently inactivates bacteria without harm to exposed human skin. This is because far-UVC light cannot penetrate even the outer (non-living) layers of human skin or eye, due to its strong absorbance in biological materials. However, because bacteria and viruses are of micrometer or smaller dimensions, far-UVC can penetrate and inactivate them. Far-UVC efficiently inactivates airborne aerosolized viruses, with a very low dose of 2 mJ/cm2 of 222-nm light inactivating >95% of aerosolized H1N1 influenza virus. Continuous very low dose-rate far-UVC light in indoor public locations is a promising, safe and inexpensive tool to reduce the spread of airborne-mediated microbial diseases. Far-UVC light is also able to penetrate and inactivate viral, bacterial, and fungal cells in a matter of seconds, which is much faster than UVC lamps.
Pressurization and air flow
Pressurization techniques may be employed to minimize the risk of outside contamination that is not carried in with people or materials. Installation of airlocks or active pressurization controls can make the workplace positive with respect to adjacent spaces.
Healthcare and BSL facilities utilize increased airflow to maintain cleaner spaces. According to the Guidelines for Design and Construction of Hospitals and Outpatient Facilities as published by The Facility Guideline Institute (FGI), infectious-disease rooms require 2 air changes per hour (ACPH) of outside air and 12 ACPH of recirculated air. The elevated air changes are implemented to capture and contain contaminants with proper filtration. A similar approach may be applied to the office workspace, provided the air systems are sized to accommodate the increased airflows.
For systems with demand ventilation controls, these controls should be deactivated (during this crisis period) to maximize the amount of outside air ventilation introduced into the spaces.
HVAC systems that introduce outside air may be operated for longer periods to increase the time that the spaces are occupied for multiple shifts and to flush them with fresh air. Application of frequent cleaning procedures within the workplace will release chemicals into the air. The implementation of flush-out cycles will capture and dilute the air within the workplace prior to workers returning the following day. During unoccupied periods, the amount of outside air may be increased beyond minimum outside air setpoints. If interior conditions (temperature and relative humidity) are relaxed during this flush-out period, it will be possible to further increase the amount of outside air during peak cooling and heating months. Depending upon existing controls in place, it may be possible to enact automatic controls and setting of outside air volume, based upon monitoring interior conditions during these unoccupied period flushing cycles, by simple reprogramming of the control sequences. For higher risk-communal spaces, it is prudent to operate these systems continuously – 24 hours a day.
Humidification
Humidification should also be considered to help minimize the spread of contagions. As noted by Dr. Stephanie Taylor, (MD, M Architect, ASHRAE DL) at a Tri-State HVAC conference, humidity above 40% inactivates almost 80% of viruses within 15 minutes. Humidification introduced by steam injection is a logical choice, but other methods, such as ultrasonic or spray injection, may be explored if sanitization of the system is maintained. Systems that rely on maintaining standing water are not recommended. Since the majority of office HVAC systems may not utilize humidification, these systems would need to be retrofitted, which would include a clean water source, a unit coupled with energy to heat to inject moisture, and a distribution method – either by injection into a duct system or the use of area humidifiers that inject moisture directly to the occupied spaces.
Sanitizing ductwork
Ductwork systems may be sanitized with aerosol sprays of disinfectant solutions or UV lamps as shown in Figure 2. UVC lamps allow for continuous sanitization of the duct systems when properly applied, while aerosol cleaners would be applied during unoccupied hours to neutralize coronavirus that may be trapped within the ductwork system. During treatment by aerosol disinfectant solution, outside air would need to be closed to allow 100% recirculation of the disinfectant to minimize dilution and increase its effectiveness. This application may not be desirable for systems that are shared between multiple tenants since treated airflow will be circulated through all spaces. Therefore, the use of UVC lamps may be more attractive for systems shared by tenants.
Air purification
Another option to increase air changes within a space while treating the airflow is the use of multiple air purifiers. These provide the ability to increase air changes when the existing HVAC systems are unable to increase airflow. In addition, these portable units may include several of the technologies previously noted, such as HEPA filtration, antimicrobial coated filters and air ionization. Portable units are easier to deploy and may be moved as need to accommodate changes within the workplace.
Applications of these technologies may be applied to various HVAC systems serving the workplace. Implementation of specific measures should be considered with goals, expectations and the specific systems to be applied, including:
- Centralized VAV systems
- Systems that recirculate air locally, such as VRF, fan powered boxes (FPB), fan coil units (FCU), and DOAS FCU
- Chilled beams
- PTAC and VTAC
- Induction units
- Baseboard heating.
Plumbing solutions
Since coronavirus may be transmitted through respiration, touch and fecal-oral transmission, restrooms will require special attention. Though surfaces may be cleaned as previously noted and HVAC systems enhanced, additional measures are recommended to maintain functional restrooms for the workplace staff. The following strategies may be applied:
- Far-UVC or UVC lamps under lids of water closets. For water closets without lids, lids would need to be added.
- Spray disinfectant applied to bowl of water closet during and after each flush.
- Use of personal toilet paper.
- Far-UVC or UVC lamp to disinfect stall after each usage.
- Hands free toilet fixtures.
- Adopt procedures to minimize the dispersion of the virus in the restroom, such as limiting use of stalls with adjacent occupancy and closing lids when flushing toilets.
- Far-UVC or UVC lamps in lids of waste bins.
- Utilize a bathroom attendant to wipe down all fixtures after each person uses the facilities.
Recent research findings now indicate that COVID-19 is not being found in water supplies.
Technology solutions
When we return to the workplace, the ability to maintain a safe distance while still working collaboratively requires technology support. In critical environments or those with close-quarters working conditions, detecting staff who may be ill and reducing contact with common surfaces like badge readers or door hardware are important.
Consider the following upgrades or modifications to existing technologies:
- Access control – Install non-contact badge readers allowing for touch-less entry of restricted spaces
- Surveillance – Install radiometric body temperature measurement cameras* for non-contact measuring of visitors or staff with significant physical support requirements.
- Wi-fi and network capabilities – With a mix of local and remote staff, network traffic will increase as remote collaboration platforms are used heavily within the workplace, even with communicating to others in the office to maintain social distancing.
- Remote collaboration – Meeting spaces should connect to the collaboration platforms fully adopted during the remote working period. (At Bala, for example, we abandoned two of the three platforms we used to use and are now optimizing our spaces for the remaining platform.)
- Business continuity – Maintain the high level of remote work capabilities required in preparation for future “circuit-breaker” quarantine measures that require temporarily moving back to remote work during outbreaks.
- Training & adoption – With the increased adoption of collaboration technology that most companies are experiencing, continuing to use those technologies and improving the effectiveness of the platforms will require ongoing training and process improvement. Expect adoption to slip when reentering your workplace and adjust feature sets and educational materials as staff come to understand the limitations of social distancing within the workplace. Managed correctly, remote collaboration systems can be equally as effective for the long term as they are now.
*Thermographic cameras may be used to screen persons when entering facilities to help reduce the likelihood of infected persons entering the spaces and spreading the virus. These cameras can be deployed for ceiling-mounted or standalone operation. However, environmental factors can greatly affect the accuracy of these devices. Guidelines for distance, number of persons being scanned, and other calibration factors must be followed.
Controlled access
The primary source of the coronavirus entering the workplace is people. As a result, the most effective method is to control access to your space and adopt other methods similar to clean room design practices, mainly for barrier control.
The number and types of barrier control necessary will be influenced by the type of building, urban versus rural environment, and access of the general public such as a building with interior retail space. Barrier controls may consist of the following:
- Single controlled access point for personnel entry. For multi-tenant buildings, it may be necessary to create one for the building and additional points for entry into each tenant space.
- For buildings that allow general public access, such as interior retail space, it may be necessary to create staff access points that are separate and distant from the general public.
- Controlled access for materials. These may be separate from personnel or shared with limitations.
- Airlock – Simple vestibule with doors interlocked to prevent simultaneous opening and to control pressurization.
- Air shower – Airlock with air at high velocity forced downward to blow potential contaminants from materials as well as people and their clothing. Alone, this will not be effective in that it will remove larger particulate that the virus may cling to but will not result in 100% removal of the virus from surfaces that it comes into contact with.
- Disinfectant spray or wipe down – Airlock with decontamination process similar to BSL or potent compound facilities, but with less stringent chemical treatment
- Pressurization – The workplace should be under positive pressure with respect to adjoining areas. This was explored further within the HVAC section.
- Screening of personnel entering the workplace, such as measuring for body temperature and turning away anyone experiencing a fever.
Some barrier control solutions require careful coordination and adherence to life safety codes. For example, if you create a single access point for a building secondary access points will need to be converted to exit only, self-locking type to maintain egress.
Based on current CDC recommendations to maintain 6 feet separation, queue lines for entry points may need to be used with appropriate spacing to relieve congestion at entrances. Another measure to consider is staggered start times for staff. If visitors are permitted, their access should be delayed until after all staff have entered, and material deliveries should also follow this schedule.
Because the virus can survive on packages and materials, these should be wiped down with sanitization solution. This procedure will require space and time to process receipt of materials. Assuming materials will enter through a common loading dock of a multi-tenant building, preliminary steps such as fogging shipments in small contained spaces with disinfectant may help, but tenants will need to take responsibility and steps to disinfect their materials, since wiping down containers will not clean the contents.
The more aggressive access control types may be warranted for buildings with less restrictive personnel requirements due to the nature of the work performed. Note, the application of controlled access will be more effective if access is limited throughout the normal workday. Therefore, it may be necessary to seclude people inside the barrier created at the building level or each tenant space for the entire day, like isolation practices being employed in the home.
Separation within the workplace
Since people may carry the virus without showing symptoms, the virus may still enter the workplace even with controlled access points. Therefore, it will be necessary to take additional precautions to minimize the spread of the virus. As such, people and surfaces remain as significant sources. The following measures may be employed to minimize risk and spread of the virus:
- De-densify people, similar to the current social distancing protective measures that have been recommended:
- Spread out seating
- Shift work
- Work remotely
- Limit or eliminate in person conference meetings
- Limit or prohibit visitors.
- Limit or avoid access to common points of congestion and contamination, such as toilet rooms, pantries, vendaterias, kitchens, and dining rooms.
- Employ mandatory PPE, including masks. Additional measures such as gloves or protective gowning may be deemed necessary on a case by case basis depending on the work performed and potential for increased risk of contagion.
Reducing the density of staff will be challenging to implement with current spaces since past trends have been to densify the workplace. The typical office furniture layouts are cubicle, fixed furniture based and will be difficult to separate. Flexible office layouts will be more accommodating in that the furniture may remain with people spread out.
To accommodate less people in the same area, it may be necessary to consider shift work as well as remote working. Implementing shift work will optimize use of available space, minimize direct contact between staff and reduce congestion at controlled access points. Note, applying shift work will require overall longer workdays for the office, and leased spaces will need to be negotiated with the landlord to allow HVAC systems to operate longer hours.
In addition, the maximum number of hours permitted may depend upon time needed to clean and wipe down all surfaces within the workplace every day. Once the maximum number of workday hours is determined, the work force may be divided into an appropriate number of groups that will be accommodated by the available space within the determined time frames for each shift. Since the shifts necessary to meet distancing requirements may require shift durations less than the typical workday of 8 hours, it may be necessary to ?allow staff to complete routine tasks from home each day. Since people are accustomed to working remotely during the self-quarantine, this should be easy to implement. Since functions reserved for conference rooms, dining rooms and other large congregation areas should presently be avoided, it may be possible to convert these spaces into temporary workspaces for the duration of the crisis.
Personal protective equipment (PPE)
Since people are the primary source of the virus and they may be infected without presenting symptoms, it is recommended that PPE be applied based upon the nature of the work performed. Examples of PPE include gloves, goggles, face shields, face masks, and respiratory protection, when appropriate. During an outbreak of an infectious disease, such as COVID-19, recommendations for? PPE specific to occupations or job tasks may change depending on geographic location, updated risk assessments for workers, and information on PPE effectiveness in preventing the spread of COVID-19. Employers should check the OSHA and CDC websites regularly for updates about recommended PPE.
In many environments wearing a standard face mask will reduce the risk of further spreading the virus. Standard masks will keep droplets from leaving a person’s mouth during normal talking, breathing and sneezing. To facilitate staff compliance, companies/tenants may need to provide these masks so that all staff wear them, as well as have spares on hand for permitted visitors and staff that forget or lose their masks.
Cleaning the workplace
Once access is controlled and the potential spread of the virus is minimized, it will still be necessary to clean and disinfect the workplace on a regular basis. Staff should be encouraged to periodically sanitize their spaces throughout the day since accidental contamination may occur from people who are unknowingly infected, imperfectly fitting PPE, improperly disinfected materials, etc. However, it is recommended that each workplace be thoroughly cleaned on a frequent basis. Frequency will depend upon measures employed to reduce contamination. The following actions are recommended:
- Sanitize spaces and all surfaces.
- Wipe and disinfect desks and workspaces, including keyboards and other office utensils that are handled daily.
- Wipe all packages and mail. Open packages and sanitize contents within as well.
- Wipe all doors and handles.
- If communal spaces such as conference rooms, pantries, pantries, vendaterias, kitchens, and dining rooms remain in operation, then these spaces should be cleaned more frequently throughout the day and possibly after each use.
- Due to the increased risk of transmission, special care shall be taken to disinfecting restrooms, including all fixtures, toilet paper dispensers, toilet paper, etc.
- Utilize UV systems, similar to those used in the airline industry, to clean office spaces overnight.
- Use sanitizing misters at the entrances to the spaces.
Conclusion
Each day we learn more about the COVID-19 virus, how it behaves, and the best recommendations and strategies for dealing with it. We will continue to monitor and evaluate this information to present our latest insights and approaches on this matter. Our goal is to help you prepare your buildings for the safe and productive return of the workforce.
This article originally appeared on the Bala website.



