Building design and operations need to consider infection control technologies in the wake of the COVID-19 pandemic
The recent spread of the pandemic coronavirus (COVID-19) has brought several new questions to the forefront with respect to the design and operation of the buildings in which we spend much of our time, specifically when it comes to infection control.
Many of us are asking “how clean are our buildings, really?” and, “what can be done to control the spread of viruses in a high-density space?” Topics like surface cleaning and air purification practices that were once the sole domain of the healthcare industry are now top of mind in discussions about workplaces, restaurants, education facilities, retail spaces, and grocery stores. With this renewed interest comes a new market for many high-quality sanitation and air filtration products – but separating the valid claims from the noise can be difficult.
In this article, we’ve summarized some of the more effective existing technologies for infection control in buildings. We’ll briefly discuss how each works along with some of their risks and benefits. There’s a variety of technologies that can play a role in reducing the potential for the spread of infection within a building, and as your partner, we at Henderson stand ready to help you select the correct technology to suit your specific application.
HEPA filtration
A standard air HEPA filter looks and acts much like any air filter in that it captures but does not kill contaminants. The HEPA designation means that the filter assembly was designed and tested to capture 99.7% of particles in the air passing through it that are .3 microns in size. The .3-micron size represents the most difficult particle size to capture so the 99.7% capture rate actually represents the worst-case efficiency of the filter. For particles that are larger or smaller than .3 microns, the capture rate increases.
Since most viruses are less than .3 microns, HEPA filters can be very effective in capturing and removing viruses from air streams, as long as they pass through the filter. However, because HEPA filters are typically installed in the ductwork and therefore must rely on the room airflow patterns to carry contaminants to the filter, small particles like viruses circulate in the room for an extended time before eventually making their way to the filter for capture. In general, while highly effective and reliable, an in-duct HEPA filter is more appropriate in preventing cross contamination between spaces than it is in guaranteeing removal of contaminants from a given space.
Advantages:
- Proven technology, no moving parts, easily retrofitted
- Effective at particle entrapment
- Effective at protecting space-to-space contamination
Disadvantages:
- Only captures particles from the ducted air – not within the space
- Some increase in energy usage due to increase air pressure drop and motor work
- Increased maintenance due to filter replacement
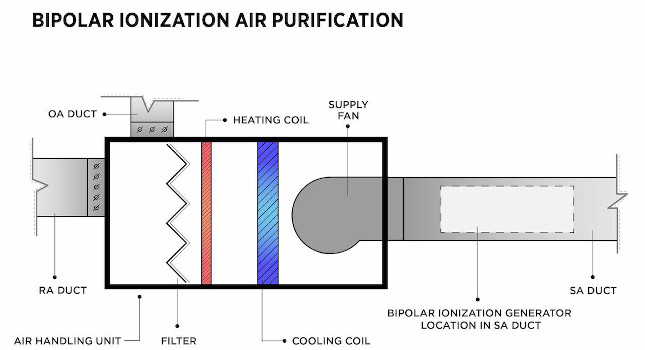
Bipolar ionization
Bipolar ionization generators create positively and negatively charged oxygen ions which bind to contaminants in the indoor air, either causing them to drop out of circulation in the room or to be captured by a mechanical filter within an air handling unit. When properly installed, operated, and maintained, bipolar ionization systems can reduce dust and mold, capture odors, reduce VOCs (volatile organic compounds), and reduce viruses and bacteria in the air.
Ions generated by these devices typically have a relatively short lifespan, so it’s important to regularly pass room air over the ion generator to ensure sufficient contact. Typically, bipolar ionization generators are installed in the ductwork or directly in the air handling unit, but recirculating room units are available through some manufacturers. With any ionization product, it is important to investigate the potential to create ozone, which has proven negative effects on human health, as a by-product of operation.
Advantages:
- Little additional pressure drop added to system
- Requires no re-engineering of existing HVAC system
Disadvantages:
- Emitter wear and calibration requirements
- Only captures particles from the ducted air – not within the space
- Potential to create ozone by-product
Active particle control devices
Active particle control devices perform similarly to a bipolar ionization generator, with one important distinction. Rather than charging oxygen molecules to act as a contaminant attraction device, active particle control devices charge the contaminant particle itself, causing it to aggregate with other smaller particles to form a larger conglomerate particle that can be captured by a downstream air filter. These devices effectively increase the filtration ability of the downstream filter by grouping smaller particles together.
Advantages:
- Little additional pressure drop added to system
- Requires no re-engineering of existing HVAC system
Disadvantages:
- Emitter wear and calibration requirements
- Only captures particles from the ducted air – not within the space
- Potential to create ozone byproduct
Humidification
Pathogens and infectious droplets travel further in dry air, especially when the relative humidity is below 40%, which is partly why we tend to see more illness in the drier winter months. By maintaining indoor relative humidity between 40–60%, building operators can reduce the risk of spreading airborne infectious diseases in their facilities. In most climate zones across the U.S., maintaining this range requires not only the dehumidification technologies that are traditionally designed in HVAC systems, but also the less common technologies that add humidification to spaces.
Advantages:
- Creates a less hospitable building climate for viruses
- Reduces static
- Increases occupant comfort in winter
Disadvantages:
- Does not capture or kill pathogens
- Consumes water for humidification
- Can add significant cost to the system installation
Ultraviolet (UV) sterilization
Anyone who has ever gotten a sunburn is familiar with UV light’s ability to degrade organic materials. Given the proper contact time and intensity, UV light can inactivate viruses and bacteria – rendering them harmless. UV lights can be installed in an air handling unit or even directly in the space itself, but the light must directly contact the pathogen in order to be effective. There is no travel distance or “conditioning” of the air that takes place.
UV light, with a wavelength between 200–280 nm has proven to be the most effective for infection control while inflicting minimal damag to human skin or other mammals present in the space. There are many novel applications of “in-room” UV sterilizers specific to almost every application, including stationary lights or portable devices mounted on robots for off hour surface sterilization.
Advantages:
- Can destroy microorganisms like mold, bacteria, and germs
- Applicable in a room-based or air handler-based setting
Disadvantages:
- Does not filter contaminants from the space
Vaporized hydrogen peroxide injections
On the more aggressive end of the spectrum for room sterilization technologies is the injection of vaporized hydrogen peroxide directly into the space. Hydrogen peroxide is a potent sterilizing agent that has been used to decontaminate buildings infected with a range of biological contaminants from anthrax spores to exotic viruses. The process is performed by injecting vaporized hydrogen peroxide into a sealed vacant space and is usually used more as an intentional sterilization procedure rather than a routine part of normal building operation.
Advantages:
- Highly effective at destroying microorganisms like mold, bacteria, and germs
Disadvantages:
- Not practical for wide disinfection of occupied/finished spaces like office buildings or schools
- Room temperature and humidity require tight controls for efficacy
- Requires pre-cleaning of all surfaces before disinfecting
Elevated body temperature detection
One way to control the risk of infection in your facility is by detecting potentially contagious patrons before (or as) they walk through your doors. To do this, one widely discussed solution is the application of thermal imaging to detect elevated body temperatures. These systems work by using infrared radiation to evaluate temperature differences on the surfaces of the skin or other materials. A variety of devices exist with this technology including ceiling/wall-mounted cameras, handheld thermal imagers, or devices integrated into existing security or building automation systems.
Advantages:
- Passive devices that can be integrated into existing systems
- Real time feedback on potential infected occupant entering the building
Disadvantages:
- Potentially slows down building entry which could complicate social distancing
- Can be expensive to administer at multiple access points
As a society, our awareness of how quickly potential pathogens can spread has increased dramatically in just the span of a few months. We understand the importance of human health, and furthermore, we understand that our economic livelihood as individuals, as a nation, and even as a world depends greatly on our ability to move about freely without concern for the spread of infection.
While safety and comfort have always been priorities for those who design and operate the buildings in which we live, work, and play, the COVID-19 pandemic has added another factor to be considered. However, with the proper application of active infection control technologies like those listed here, we are confident we can meet this challenge head on to help us all get back out in our communities as quickly as is safely possible.
This article originally appeared on Henderson Engineers’ website. Henderson Engineers is a CFE Media content partner.




