There are many changes to NFPA 99-2012. Engineers should review the code carefully to better understand how it affects electrical systems, risk assessments, and other pertinent topics.
Do the recent changes in NFPA 99: Health Care Facilities Code require isolation panels in all operating rooms?
NFPA 99-2012 has so many changes throughout the document that the committee decided to forgo the usual markers that indicate a change. Several of the code changes are relocated sections to improve organization. However, there is an obvious philosophical shift within the code.
This shift is apparent within the new text of Chapter 4 (formerly Electrical Systems). It’s apparent that risk assessment procedures are going to play a more formal role in certain code interpretations. Unfortunately, when someone asks you, “Does that meet code?” the technically correct answer is going to be “It depends on the risk assessment.”
So what does risk assessment/risk probability all mean?
NFPA 99 doesn’t give a lot of firsthand guidance on a “defined risk assessment procedure” other than giving the four categories of risk (NFPA 99-2012 Section 4.1) and a reference to ISO/IEC 31010, NFPA 551: Guide for the Evaluation of Fire Risk Assessments, and SEMI S10-0307E. These documents contain some new concepts for the design engineer to consider, which are strongly encouraged for reading.
For some reason, the average person tends to think of risk probability in terms of his or her chance of getting hit by lightning (1 in 700,000 per year, or 0.000001% chance of being hit). Even though it’s not the engineer’s role to interpret or conclude for a facility what an “acceptable” risk level is, it’s always useful to have a reference benchmark when asked “What does that mean?”
Chapter 6 is now dedicated to Electrical Systems; it’s nearly a duplicate of NFPA 99-2005 Chapter 4. However, NFPA 99-2012 Section 6.3.2.2.8.4 now states, “Operating rooms shall be considered to be a wet procedure location, unless a risk assessment conducted by the health care governing body determines otherwise.”
The appendix A.6.3.2.2.8.4 also states, “In conducting a risk assessment, the health care governing body should consult with all relevant parties, including, but not limited to, clinicians, biomedical engineering staff, and facility safety engineering staff.”
Depending on your personal bias, this is clear and conclusive proof that:
- All new operating rooms should be considered wet locations and as such should be equipped with an isolated power system, OR
- Isolated power systems are not required in any new operating rooms, as long as the facility performs a risk assessment and that the risk is relatively low.
Engineers typically stick to the facts, but it’s worth stressing that there is a great deal of debate about this change in the code.
What is a wet location?
The American Society for Healthcare Engineering (ASHE) has come out with a statement clearly articulating its objection to classifying all operating rooms as wet locations (see their white paper titled, “NFPA 99: How to Conduct Operating Room Risk Assessments”). ASHE relates the ongoing struggle on this issue back to 1970 and articulates a general methodology for conducting a risk assessment based on empirical measurements of existing operating rooms. Unfortunately, most engineers do not have access to an existing operating room for empirical testing. If you have a fully engaged owner/client, this is a good document to read.
There is also a well-written article issued by the Fire Protection Research Foundation, “Operating Rooms as Wet/Dry Locations Risk Assessment Project” (Brenton Cox, PhD, Exponent Inc., 2012). The article does a good job of identifying a mathematical model for the general terms outlined in NFPA 99.
Since most consultants are conservative and risk averse, the majority will gravitate toward conclusion Number 1 described above. However, like all things in our profession, it’s not going to be that simple. As clients become more cognizant of this issue, they will start asking, “Do I really need isolated power in all of my operating rooms?” or “I spoke with my colleague and he doesn’t have isolation panels, why do I need them?” or “Can you perform a risk assessment for me?”
Because I’ve been down this road, I’m going to share with you what I’ve learned and how you can use it with your clients.
Steps to complying with NFPA 99
1. Start by stressing that this is not an engineering responsibility.
As engineers, we are traditionally “the smartest person in the room,” and as such, we are big targets for logical analysis and ultimately complicated math projects like this, usually without compensation. The engineer most likely has a role in the risk assessment process, but the effort is fruitless until a risk assessment team, including the folks mentioned in NFPA 99, is assembled.
NFPA specifically lists clinicians, biomedical engineering, staff, and facility safety engineering staff as required to be on the team. This group is going to be the source of the data that you’ll use to calculate the risk probabilities. I kept the group that I worked for accountable for supplying the data that I used in the calculations. Why is it necessary that the engineer perform the calculations? Reference the first sentence in the previous paragraph.
2. Lead the meetings, and ask the questions.
In my experience, this is an iterative process. The clinicians, biomedical engineers, etc., that I’ve worked with are normally confused as to why they are even participating in this process. As such, they will not arrive at the first meeting with suitable information that you need to perform the calculations. Set up a weekly conference call that lets the team get used to running down the data that you will need.
3. Explain why it’s different this time.
Participants often say, “It’s a general operating room! What else do you need to know?’’ Explain why we are doing the assessment and how much of the risk is driven by the number/types of medical procedures that will be performed in the room. The nursing/scheduling staff normally can give you a comprehensive list of the procedures with relative frequencies for an operating room (it is their business).
4. It’s all about fluid dynamics.
The biggest unknown and ultimately the largest risk factor is directly proportional to the quantity of fluid that can end up on the floor. Understand the fluid impact for every procedure. Questions to ask include:
- How much (measured in milliliters) fluid do you use when you irrigate a cysto procedure?
- When fluid is spilled, how much is spilled?
- Do you have a special irrigation table?
- Do you use special draping?
Are there inherent advantages/disadvantages to the electrical system the engineer has designed? Are there any cords on the floor? Have any of the cords been altered or require adapters? (These are all past reasons for reported microshock incidents.)
5. Give the team homework assignments.
Everyone is programmed to fill out forms. Table 1 is an example of the worksheet used recently. This helped the staff understand the needed information in an easy format.
6. Crunch the numbers.
Once the team has provided the basic information for the operating room procedures, it’s time to convert the data into something useful for the actual risk assessment portion of the exercise. The actual risk is directly proportional to the “pool” size on the floor. Using a linked Microsoft Excel sheet, it is easy to develop the information in Table 2.
7. Develop a fault tree.
The culmination of all this work is expressed in a fault tree. Table 3 shows an example.
8. Calculate risk results.
Table 1: Risk worksheet
Table 2: Risk assessment (calculating event per year)
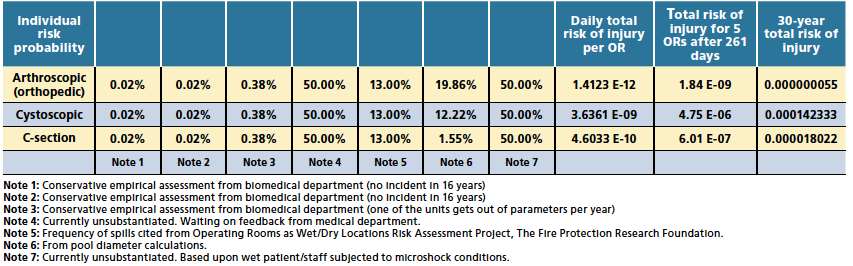
Table 3: Risk assessment (calculating event per year)
Finally, combine all the information into an aggregate risk probability that is suitable for the published results of the risk assessment team that can be included in the final published report (by the facility) that will be reviewed by the hospital executive board as, eventually, the authority having jurisdiction.
Reviewing the results in Table 3, it looks like the chance of having an undesirable electrical result for either an arthroscopic or C-section procedure over a 30-year period is far less than a person’s chance of getting hit by lightning any given year. However, using the risk assessment, there is s a better chance of having an undesirable event (i.e., microshock) with a cysto procedure (over a 30-year period) than getting hit by lightning. This result isn’t surprising because a cysto procedure is a known “wet” procedure and often is considered the benchmark for when to install an isolated power system.
Interpreting and applying the code will be unique for each situation. It’s always better to err on the conservative side when lives are at stake; but realize that the code writers appear to be evolving away from a prescriptive solution for many high-risk installations. As engineers, we often speak to the client about the relative costs, lead-time, installation method, on-going maintenance, etc. for a proposed engineered system. We will be compelled to address the associated risk in that conversation wherever NFPA 99-2012 has been adopted.
Gerald Versluys is a senior electrical engineer and principal at TLC Engineering for Architecture. His areas of expertise include sustainable health care design and campus distribution systems. He is a member of Consulting-Specifying Engineer’s editorial advisory board.