There are many ways to improve indoor air quality in buildings and to address COVID-19 fears

Learning Objectives
- Learn evidence-based steps for improving indoor air quality.
- Define the three primary modes of COVID-19 transmission.
- Describe at least two control strategies to improve indoor air quality.
The U.S. Environmental Protection Agency has ranked indoor air pollution among the top five environmental danger facing the general public. With Americans spending up to 90% of our time indoors, indoor air pollutants making indoor environments more toxic than outdoor environments. With building envelopes being constructed even tighter, it becomes clear that exposure to harmful indoor pollutants must be addressed.
Indoor air quality concerns for all building types have moved front-and-center with the arrival of COVID-19. Myriad shifting and competing scientific positions surrounding transmission of COVID-19 — along with various heating, ventilation and air conditioning products to combat the virus — have hit the market in record time.
Studies are in progress as scientists are learning more about how the disease is transmitted and contained. As building owners and occupants juggle competing priorities with ongoing occupancy and reoccupancy of buildings, smart, practical and layered solutions are the ones that are proving to win out in the battle to manage indoor air pollution.
Taking a step back, COVID-19 is one of a number of viruses belonging to the class of biological pollutants within the broader category of indoor air pollutants. It’s important to remember an indoor space can experience pollution not only from substances such as the COVID-19 virus, but also bacteria, mold, radon, dander, pollen or smoke. Additionally, industrially produced substances such as volatile organic compounds and chemicals are classified as indoor pollutants.
Indoor air quality
The goal with all IAQ concerns is air free from harmful pollutants, what can be termed a “zero-pollutant building.” Though in practical terms a building will likely contain some level of pollutants, a zero-pollutant building does not contribute adverse health effects to the occupants. EPA indoor air quality refers to the air quality within and around buildings and structures, especially as it relates to the health and comfort of building occupants.”
No matter the contaminant it is useful to follow the following pragmatic steps for remediation. The path to healthy indoor can be achieved by:
- Limiting time in buildings.
- Physically removing sources of contamination.
- Cleaning surfaces.
- Improving ventilation.
- Filtering the air.
- Cleaning the air.
These six steps will next be put into action to combat the indoor air pollutant currently top of mind: COVID-19.
Virus transmission
It is known that viruses can be transmitted in three main ways. The first way is through human contact with animate or inanimate objects that are contaminated with the virus. These objects are known as fomites. The U.S. Centers for Disease Control and Prevention has ruled that fomites are not a major source of COVID-19 transmission due to the lipid envelope structure of the virus, something on the order to 16% to 25%.
The second method of transmission is through droplets, which are larger particles that fall to the ground after being expelled from the mouth or nose.
The third method of transmission is aerosol, which is made of particles so small they float in the air for a time after being expelled. As documented virus infections continue to rise, aerosol transmission is increasingly being accepted as the dominant form of COVID-19 transmission, similar to previous discoveries made for diseases such as tuberculosis, measles and chicken pox. Physical and mechanical methods are required to “treat” COVID-19 in airstreams.
Experts in the academic scientific community have been worrying that the CDC is not being helpful enough in its guidance and air quality recommendations around COVID-19. Now that it is generally accepted that COVID-19 is airborne, it is helpful the CDC has recently confirmed this fact on its website. This means the virus that causes COVID-19 can float in the air in aerosol form, like smoke particles hover for a time.
In indoor environments, the aerosol can linger longer — and longer still in poorly ventilated indoor spaces. In such a case, the virus can spread farther than 6 feet from a source, well beyond the minimum social distancing distance. For this reason, poorly ventilated indoor spaces need to be addressed as high risk for health concerns from COVID-19.
The size of aerosols versus droplets is a source of debate, though the general consensus about particle size lays in the 0.1 to 100 microns range for both, with droplet in the larger part of the range. If droplets are defined as particles that fall to the ground within 6 feet and are also visible, that definition can still pose an issue because distance traveled will depend on the velocity of the expelled particles.
For example, a person is sneezing or talking will determine the distance of travel of a particle of the same size. This brings us back to one fact that is not up for debate: Poor air exchange can prolong the time that aerosolized particles can remain airborne.
Mitigating virus transmission
When talking about mitigation of virus transmission indoors, there are several actions that can be taken that follow the path to healthy indoor air. It’s important to note there are no completely safe public indoor environments during the pandemic no matter what actions are taken, however risk of exposure can be greatly reduced.
Step 1: Limit the source
First, take actions that limit the amount of virus in the air. These actions serve to limit the source. To achieve this, begin by limiting the amount of people in the building. Have those that are in the building adhere to close-fitting mask wearing and social distancing. This is why officials moved to requiring reduced capacity in restaurants and office environments that remain open during the pandemic. Another action is limiting more active activities that can produce more airborne particles, such as shouting and vigorous exercise.
Along with the above actions, housekeeping and wayfinding are important. Keep a sanitized environment disinfecting surfaces contacted by multiple people and limit or close use of shared facilities within the building. Arrange travel within the building to maximize distance from person to person and contain areas of the building that are not well ventilated.
Step 2: Reduce concentration
Second, it’s important to further address ways to reduce the concentration of virus in the building. This also holds true for any indoor pollutant. One important way to accomplish this is to increase the amount of outdoor air entering a given space through ventilation strategies. This can be through open windows and doors as long as outdoor air contaminants and air temperature and humidity conditions are not themselves unhealthy. Use fans and air circulators to speed up the exchange of air through windows and external doors.
Source capture can also be a useful strategy; for example, exhausting potentially densely populated areas such as reception or waiting areas and negatively pressurizing such areas with respect to the rest of the building. Scientists don’t yet have a specific quantity on what represents a dangerous level of infectious concentration of virus in the air.
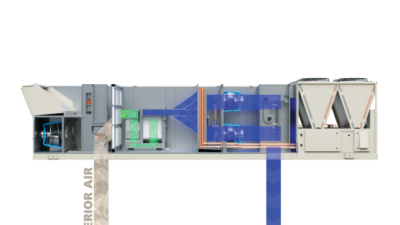
Increase ventilation air volume being brought in through ducted intakes into the building mechanical systems. As a general rule, most HVAC systems with direct expansion cooling can handle roughly 25% outdoor maximum. The objective is to ventilate spaces and do not leave outside air dampers shut. Six air changes an hour is an ideal baseline target for such air exchange; five air changes represents a good target. As a comparison, a typical rooftop unit or split systems with 25% outdoor air provides around 1.5 air changes per hour, so most buildings are a long way off from this target.
Filtration of airflow in building HVAC systems is another method of trapping viruses and pollutants. Filters have various ratings defining their ability to trap particles of different sizes. The most popular rating in use today is the MERV rating. MERV measures the performance of filtering particles in the 0.3- to 10-micron range.
As a comparison, the size of the COVID-19 virus is 0.125 microns in free form, however COVID-19 attaches itself to larger particles and does not typically exist in its free form. Organizations such as ASHRAE recommend upgrading air filters in HVAC systems to the highest efficiency possible that is compatible with the system and checking the filter fit to minimize filter air bypass.
Aim for a filter with a minimum MERV 13 rating or higher if possible. A MERV 13 filter has an efficiency of roughly 90% of particles in the 3- to 10-micron range, 85% of particles in the 1- to 3-micron range and 50% of particles in the 0.3- to 1-micron range. To extend the service life of a MERV 13 filter, a prefilter of a lesser MERV rating should be installed upstream if possible.
Beyond MERV rated filters exist the high-efficiency particulate air filter. HEPA is another of the pleated mechanical filters. They are required to have a minimum removal efficiency of 99.97% on particles 0.3 microns in size. Other particle sizes are trapped with higher efficiency within the HEPA filter. In-line HEPA filters will typically not work on an HVAC system not designed for them due to the high pressure drop imposed on the system. Bypass-type HEPA filters are a workaround that can be used on some mechanical systems, space permitting. These are filters that have their own fan systems and circulate and filter typically a portion of the total HVAC system airflow.
Filtration plays a role in overall virus risk mitigation. However, similar to all the solutions presented here, filtration is not a solution by itself. It must be combined with other measures to build on its beneficial effect.
Another approach to filtration and air cleaning is consideration of using portable air cleaners, also termed “air purifiers.” The most effective class of these air purifiers has HEPA filters to supplement increased HVAC system ventilation and filtration, especially in areas where adequate ventilation is difficult to achieve. Directing the airflow so that it does not blow directly from one person to another reduces the potential spread of droplets and aerosols that may contain infectious viruses.
Portable air cleaners may be helpful when additional ventilation with outdoor air is not possible without compromising indoor temperature or humidity comfort or when outdoor air pollution is high. For an air cleaner to be effective in removing viruses from the air, it must be able to remove small airborne particles in the size range of 0.1 to 1 micron.
Like other technologies discussed, air cleaning is not enough to protect people from exposure to the virus that causes COVID-19. ASHRAE guidelines recommend using HEPA air purifiers that can provide a minimum of two air changes per hour. It is important to note that with any filter, a virus is not disabled and continues to live in the media and must be disposed of carefully. Some leading scientists advocate avoiding portable air purifier with add-ons containing ionizers or ultraviolet lights due to the potential for adverse effects of ozone.
The benefits obtained from a combined outdoor air ventilation plus portable air cleaner with HEPA filter combination are that it helps get closer to reaching the recommended levels of five to six room air changes per hour discussed previously. However, experts in the scientific research community believe that the transmission of infectious disease through HVAC systems, particularly those in nonmedical buildings, is a relatively small factor.
Step 3: Disable the virus
Once actions are taken to limit the amount of virus in the air and further ways to reduce the concentration of virus in the building are addressed, employ solutions that disable the virus. Techniques such as germicidal UV light (UVGI or UVC), ionization, plasmas and oxidation fit into this category.
UVGI has proven to be effective technology used for more than a century in disabling or deactivating viruses and can be used to supplement ventilation and filtration strategies and increase effective air change rates. In addition to inactivating virus, it can kill bacteria and mold. Applications are available that locate lighting in air handling systems shining on coils, filters and wet surfaces or in the airstream.
In-room applications are used within the occupied zone that serve to sterilize a room once unoccupied. Upper-room disinfection directing energy above the occupied zone where continuous operating is desired. One drawback of these systems is the UVC lights cannot shine on skin or eyes without causing severe burns. Thus, protection controls must be in place to insure people are not exposed with lights operating. Newer technology UVGI lighting is being developed at a lower wavelength that has the advantage that it can be shone directly on people. But it is not yet commercially viable.
Another technology gaining popularity during the pandemic is needlepoint bipolar ionization systems. NPBI operates by releasing negative and positive ions into the air that disable viruses. In-HVAC system applications using the HVAC system as the delivery method and in-room portable units are available. NPBI inactivates viruses and bacteria; kills molds and mildew; neutralizes VOCs, smoke and odors; and aids in collection of pollen and airborne dust particles. When choosing such a system, verify that they are UL 2998 compliant, meaning it does not produce harmful ozone. The units have optional sensors that can measure ion production levels and report to a building automation system.
NPBI systems have been in existence for some time as an alternate to ASHRAE 62.1: Ventilation for Acceptable Indoor Air Quality ventilation rate procedure to lower ventilation volumes using ASHRAE’s indoor air quality procedure. However, this procedure has fallen under criticism to being inadequate for acceptable IAQ because it considers a minimal list of contaminants and uses a subjective odor test. Advantages of NPBI include a more favorable cost point relative to UVC, self-cleaning and little to no maintenance. As with any system choice, proper design, installation and maintenance are required following manufacturer’s instructions.
Smart buildings to improve occupant health
Yet another frontier on the path to a zero-pollutant building is smart building technology. A smart building can be thought of as a building using data and technology to share information between building systems and optimize building performance. A smart building may also take action automatically toward such optimization.
Historically, smart buildings have focused on HVAC systems, managing energy use, building access control and lighting control integration. It is not too difficult to imagine the power of a building information and control systems being expanded to help manage occupant health through activities such as thermal imaging, managing building occupancy levels and social distancing.
Smart buildings, when designed with IAQ in mind, have a place in the war on virus transmission and improving occupant health and wellness. Smart buildings need to be employing technologies and data integration to support occupant health and wellness. New technologies and the ability to communicate across those technologies with data analytics can allow building operators and occupants the ability to optimize operations to maximize health and wellness.
Smart buildings provide more information and control for IAQ concerns. For example, carbon dioxide sensing is becoming commonplace in buildings with a BAS. BASs are being used to reduce the amount of outdoor air, thus saving energy cost, by measuring CO2 levels, a process known as demand-control ventilation. However, CO2 is a tracer for IAQ and can be thought of as an indicator of poorly ventilated spaces. One adaption of CO2 monitoring during a pandemic is the BAS can be used to notify occupants to move out of a space if the level of CO2 or other dangerous gas increases and issue a work order to investigate the potential ventilation issue.
Smart building analytics platforms also integrate data from utility companies and weather resources to reduce operating costs. With the arrival of more sources of external information system data, such as air quality alerts, virus level alerts or statistical models of rates of infection by air change, a BAS can conceivably use the data to alert operators to control sequences changes or provide notifications to building managers or occupants. This has the potential to create a healthier, safer environment for occupants. The age of COVID-19 is also being met with an accelerated shift to contactless control solutions, including access control, plumbing fixture control, app controlled or voice-activated devices.
Another useful smart control application relates to measurement of space usage or occupancy levels, even counting the number of occupants in a space. The control system can indicate space usage, space density and allocations for social distancing, and also optimize cleaning services. Control systems can be used in this manner to restrict who may enter a facility during certain conditions or limit access in specified areas.
Sequencing protocols can be used to automatically shift to alternate modes of control during the pandemic. For example, on high-alert orders from government officials, demand-control ventilation strategies can be temporarily disabled and operating schedules adjusted to provide post-purge or pre-purge strategies after or before occupancy to flush the building with outdoor air. Think of these strategies as morning warm-up or cool-down with the outdoor air dampers open.
Depending on the season and climate zone, pre- or post-purge strategies are employed to save energy by running HVAC systems during the time of day when outdoor air temperatures are least impacting energy cost. This solution is being used at the new Meeker High School project in Meeker, Colo., which opened in August 2020.
COVID-19 has sparked renewed interest in combating indoor air pollution in what may be termed the quest for the zero-pollution building. There is no one-size-fits-all solution and the solution does not lie with one stakeholder, but rather a team approach involving owners, architect, engineers, installers and manufacturers. Best results are achieved with simple, smart solutions informed by science, layering strategies to yield the largest combined effect.